
While a few ultrasound procedures suggest increased instances of patient infections due to low-level disinfection techniques, statistically, results from peer-reviewed studies do not confirm this idea.

While a few ultrasound procedures suggest increased instances of patient infections due to low-level disinfection techniques, statistically, results from peer-reviewed studies do not confirm this idea.

For terminal cleans, investigators studied the effect of UV-C disinfection added to chlorine-based disinfectants on the likelihood of MDRO transmission from the source occupant to subsequently exposed occupants.

Take 5 minutes to catch up on Infection Control Today’s highlights for the week ending July 8.

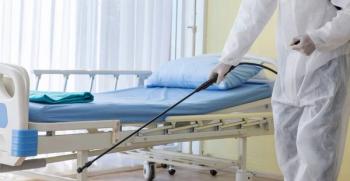
A recent study by NYU Langone investigators determined that disinfecting high-touch surfaces within patient rooms with NaDCC via wipes and electrostatic sprayers yielded lower mean bacteria colony counts.

Two patients were found with C auris in the CVAHCS beginning in October 2020, and a recent study describes how the facility handled the situation.

Take 5 minutes to catch up on Infection Control Today’s highlights for the week ending July 1.


Take 5 minutes to catch up on Infection Control Today’s highlights for the week ending June 10.

Despite the emphasis on more improved infection prevention practices, stethoscope hygiene continually falls short, possibly leading to more health care-acquired infections.

From language barriers to lack of equipment, environmental hygiene is suffering throughout the world.
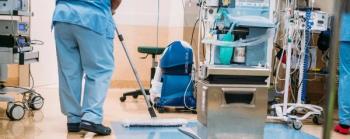
Over 50 health care facilities from 35 countries participated from both higher and lower income settings.

Take 5 minutes to catch up on Infection Control Today’s highlights for the week ending June 3.
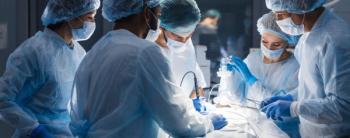
AMR and surgical site infections are a consistent issue for surgeries, and often surgeons feel they have done everything they can to reduce the risk, and yet the event still occurs with an alarming frequency. Is there anything novel that can be done? ICT® tries to find out.

How do the veteran and the novice infection preventionists work together in the present climate? What do they think are their strengths and their differences as they combine their knowledge in the health care field? Infection Control Today® asked a veteran and a novice to find out.

Take 5 minutes to catch up on Infection Control Today’s highlights for the week ending May 27.

Device-associated HAIs were likely impacted by the continued alteration of hospital practices that occurred throughout the pandemic.

To reduce the risk of surgical-site infection, utilize evidence-based interventions and give feedback to clinicians on bacterial transmission using Staphylococcus aureus as a marker.

The bugs are winning, but only because we are letting them.

Regardless of vaccination status, health care workers were protected with daily and regular hydrogen peroxide antisepsis.

However, respiratory HAVIs continued to be reported, despite elevated prevention practices, leaving young, susceptible patients threatened.

Take 5 minutes to catch up on Infection Control Today’s highlights for the week ending May 20.

Patients with home infusion therapy have improved outcomes when home health care agencies and acute care facilities communicate relevant information on their shared patients.

A comprehensive look at whether mask wearing is beneficial for both SARS-CoV-2 and other viruses spread by airborne particles and respiratory droplets.

A new comprehensive article lays out best practice guidelines for 14 areas of infection prevention and control.