Personal Protective Equipment
Latest News


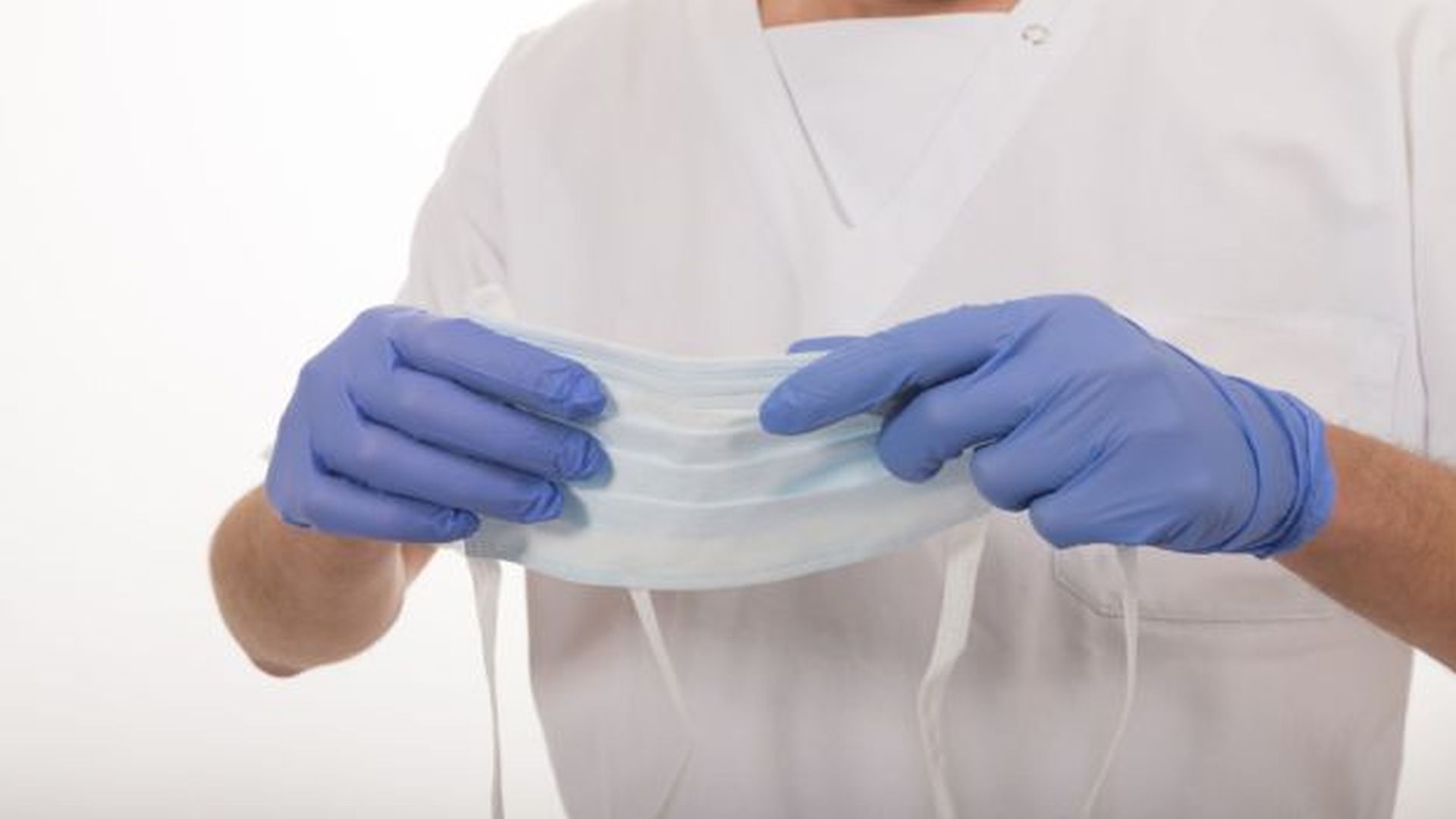
A University of Alberta engineering researcher has developed a new way to treat common surgical masks so they are capable of trapping and killing airborne viruses. His research findings appear in the prestigious journal Scientific Reports, published by Nature Publishing Group.
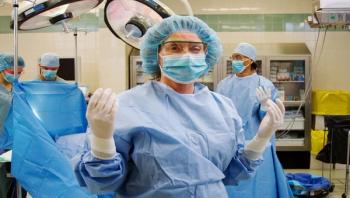

As personal protective equipment (PPE) continues to play an integral role in prevention of transmission of infection in the healthcare setting, we discover by looking back at the history of protection of healthcare workers (HCWs) and prevention of spread of infection, that the concept is several centuries old.
According to 2014 occupational incident surveillance data from nearly 30 U.S. hospitals, when an employee experiences a splash or splatter of blood or body fluid (e.g. blood or bloody urine) into the eye they are only wearing eye-appropriate personal protective equipment (PPE) 3.5 percent of the time. These mucotaneous exposures are extremely high risk. Just as the eyes are the windows to the soul, they are the frontlines for risk of disease transmission from patient to worker. If we experience fatigue, allergies, irritation, or infection our eyes become even more susceptible to microorganisms that come into contact with them.


The American College of Surgeons (ACS) has released a statement on professional attire for surgeons in and out of the operating room (OR). The new ACS guideline for appropriate attire is based on professionalism, common sense, decorum, and the available evidence.


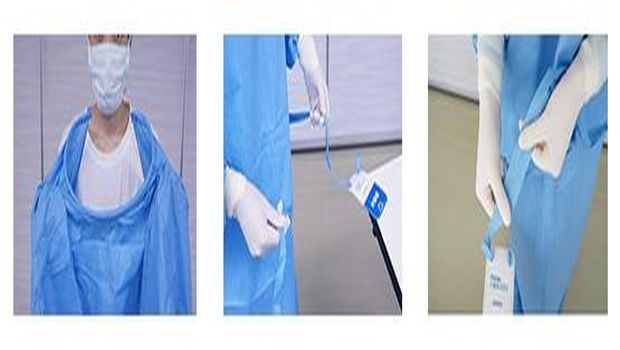
With the Ebola crisis in the rearview mirror but lurking, cases of C. difficile on the rise, and other known and emerging viruses creeping across the globe, health leaders are focusing greater attention on protecting the people on the front lines of care. The proper removal of personal protective equipment (PPE) – think masks, gloves and gowns – ranks among the most critical of those topics and it’s one infection preventionists should address with physicians, nurses and other healthcare personnel sooner rather than later. The need is pressing. Recall that Ebola infected more than 500 health workers in West Africa in 2014. Meanwhile, other professionals have contracted C. diff and MERS. Experts have not been able to irrefutably link those occurrences to improper PPE removal; however, they have enough experience to posit with authority that poor technique has played a role in at least some of the diagnoses. The reason is simple: Too few healthcare workers take off their PPE in such a way that does not pollute their clothing or skin. To wit, a recent study published by JAMA Internal Medicine showed that 46 percent of doffing simulations engendered some level of contamination.



Fewer than one-fifth of ambulatory-care nurses surveyed in a recent study reported compliance with all nine components of Standard Precautions, indicating a continuing need for identifying barriers to compliance and emphasizing patient and healthcare personnel safety. As Powers, et al. (2016) emphasize, "Exposure to blood and bodily fluids represents a significant occupational risk for nurses. The most effective means of preventing bloodborne pathogen transmission is through adherence to Standard Precautions (SP). Despite published guidelines on infection control and negative health consequences of noncompliance, significant issues remain around compliance with SP to protect nurses from bloodborne infectious diseases, including hepatitis B virus, hepatitis C virus (HCV), and HIV."


Healthcare institutions face the question of whether to use disposable or reusable medical devices. Although in certain situations one category is clearly a better choice than the other, choosing between disposable products and reusable devices is more frequently a difficult and unclear decision. Both devices are characterized by compelling pros and cons that may force healthcare facilities into a complex and multi-faceted decision-making process.



Q: Are we allowed to use latex gloves in the decontamination area? Is there any documentation in AAMI or OSHA that dictates the use of latex gloves in the decontamination area? Secondly, are we allowed to wear gloves in the sterile prep area while putting together trays?A: According to the Occupational Safety & Health Administrations’ Blood Borne Pathogen Ruling (2001), “Personal protective equipment (i) Provision. When there is occupational exposure, the employer shall provide, at no cost to the employee, appropriate personal protective equipment such as, but not limited to, gloves, gowns, laboratory coats, face shields or masks and eye protection, and mouthpieces, resuscitation bags, pocket masks, or other ventilation devices. Personal protective equipment will be considered “appropriate” only if it does not permit blood or other potentially infectious materials to pass through or reach the employee’s work clothes, street clothes, undergarments, skin, eyes, mouth, or other mucous membranes under normal conditions of use and for the duration of time that the protective equipment will be used. Accessibility. The employer shall ensure that appropriate personal protective equipment in the appropriate sizes is readily accessible at the work site or is issued to employees. Hypoallergenic gloves, glove liners, powderless gloves, or other similar alternatives shall be readily accessible to those employees who are allergic to the gloves normally provided.”



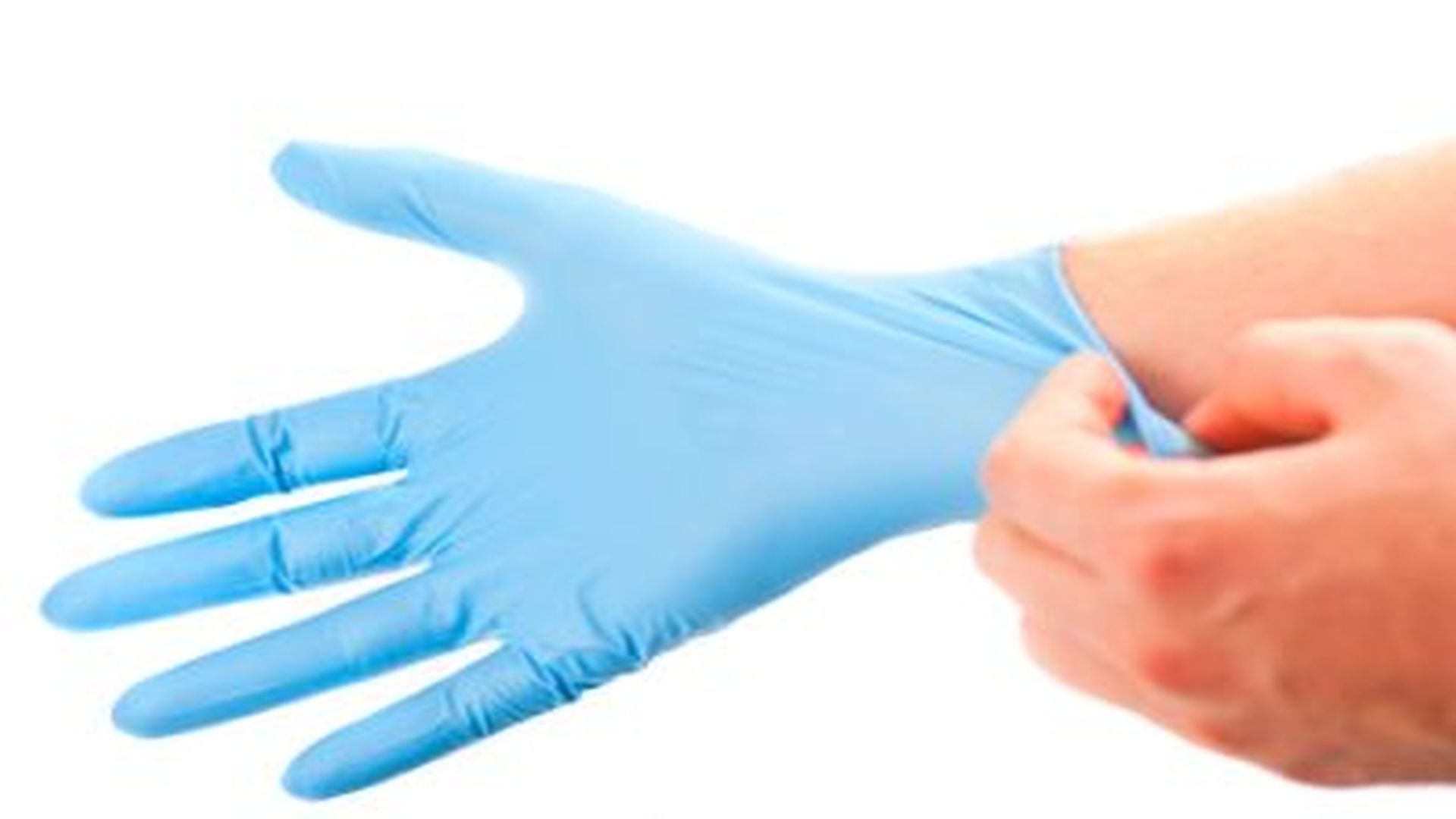
The use of disposable gloves is integral to modern healthcare. Providing a protective barrier between patients and healthcare personnel, medical gloves discourage transmission of a wide variety of diseases. Currently, several types of examination and surgical gloves are available, falling into two main categories: traditional gloves manufactured with materials that provide optimal functionality but may cause health complications, or gloves that are made with newer materials and technologies but may have deficits in shelf life, strength and elasticity.


U.S. hospitals recorded nearly 58,000 work-related injuries and illnesses in 2013, amounting to 6.4 work-related injuries and illnesses for every 100 full-time employees -- almost twice as high as the overall rate for private industry. In June, the Occupational Safety and Health Administration (OSHA) announced it was targeting some of the most common causes of workplace injury and illness in the healthcare industry, and is expanding its use of enforcement resources in hospitals and nursing homes to focus on patient or resident handling; bloodborne pathogens; workplace violence; tuberculosis, and slips, trips and falls.

Johns Hopkins University and DuPont have signed license and collaboration agreements allowing DuPont to commercialize a garment with innovative features from Johns Hopkins to help protect people on the front lines of the Ebola crisis and future deadly infectious disease outbreaks. DuPont intends to have the first of these garments available in the marketplace during the first half of 2016.